PTSD Intrusion Symptoms: Why They Happen
Learn what intrusion symptoms are, why they develop after trauma, and practical grounding strategies to manage them—plus when to seek professional support for lasting relief.
Intrusion symptoms are one of the most defining and often distressing features of trauma. For many individuals living with Post-Traumatic Stress Disorder, these symptoms can feel unpredictable, overwhelming, and difficult to control. They may appear as vivid memories, flashbacks, distressing dreams, or sudden emotional and physical reactions that seem to come “out of nowhere.”
From a psychological and neurobiological perspective, intrusion symptoms are not random or irrational. They reflect the way trauma is encoded and stored in the brain and body. In this sense, post-traumatic stress can be understood as a kind of nervous system injury, where normal processes of memory, threat detection, and emotional regulation have been disrupted (Brewin et al., 2010; Ehlers & Clark, 2000).
Understanding the different types of intrusion symptoms, how they develop, and how to stabilize them is essential for both individuals experiencing trauma and clinicians supporting recovery.
What Are Intrusion Symptoms?
Intrusion symptoms involve the involuntary re-experiencing of a traumatic event. Unlike ordinary memories, these experiences feel immediate and emotionally intense, often accompanied by strong physiological reactions.
According to diagnostic frameworks, intrusion symptoms are a core feature of post-traumatic stress and include recurrent, involuntary, and distressing recollections of the event (American Psychiatric Association, 2013). However, in clinical practice, they can take many forms that extend beyond simple memory recall.
Different Types of Intrusion Symptoms
Intrusive Memories
Intrusive memories are the most common form of re-experiencing. These are unwanted thoughts or images related to the trauma that enter awareness without intention.
They are often:
• Vivid and sensory-based
• Emotionally charged
• Difficult to dismiss
Unlike typical memories, they do not feel like something that happened in the past. Instead, they often carry a sense of immediacy, as though the event is happening again in the present.
Flashbacks
Flashbacks are more intense and immersive than intrusive memories. During a flashback, an individual may feel as though they are reliving the traumatic event.
This can involve:
• Visual or auditory re-experiencing
• Loss of awareness of the present environment
• Strong physical reactions such as increased heart rate or sweating
Flashbacks occur because the brain has not fully integrated the trauma into a coherent, time-bound memory (Brewin et al., 2010).
Trauma-Related Nightmares
Nightmares are another common intrusion symptom. These may involve direct replays of the traumatic event or symbolic representations of threat, danger, or loss.
Sleep disturbances linked to trauma are well documented and reflect ongoing hyperactivation of the stress response system (Hamilton et al., 2018). Individuals may also develop fear of sleep due to repeated distressing dreams.
Emotional Intrusions
Not all intrusions are visual or cognitive. Some individuals experience sudden waves of emotion—such as fear, shame, or panic—without a clear conscious trigger.
These emotional intrusions are often linked to implicit memory systems, where the emotional tone of the trauma is reactivated without explicit recall (Ehlers & Clark, 2000).
Somatic or Body-Based Intrusions
Trauma is stored not only in memory but also in the body. Somatic intrusions may include:
• Sudden muscle tension
• Gastrointestinal discomfort
• Rapid heart rate
• A sense of physical threat or alarm
These experiences reflect activation of the autonomic nervous system and can occur even in the absence of conscious awareness of the trauma.
How Intrusion Symptoms Develop
To understand intrusion symptoms, it is essential to examine how trauma affects memory processing and the nervous system.
Disrupted Memory Encoding
During a traumatic event, the brain prioritizes survival over coherent memory formation. The amygdala becomes highly active, signalling threat, while the hippocampus—which organizes memory into a coherent narrative—becomes less effective.
As a result, the experience is encoded in a fragmented and sensory-based way rather than as an integrated story (Brewin, 2014). This leads to memories that are vivid but poorly contextualized.
Blocked Memory Integration
Under typical conditions, memories are integrated into autobiographical memory and recognized as belonging to the past. Trauma disrupts this process.
Dual representation theory suggests that trauma is stored in two parallel systems:
• A verbal, contextual system
• A sensory, emotional system
Intrusion symptoms occur when the sensory system is activated without sufficient regulation from the contextual system (Brewin et al., 2010).
Persistent Sense of Threat
Another key factor is the ongoing perception of threat. The brain may continue to interpret the trauma as unresolved or ongoing, which can lead to persistent hypervigilance.
According to cognitive models, intrusions persist when individuals interpret the trauma in ways that reinforce danger, such as believing they are still unsafe or permanently changed (Ehlers & Clark, 2000).
This maintains hypervigilance and increases the likelihood of involuntary memory activation.
Strong Cue Associations
During trauma, neutral stimuli (e.g., sounds, smells, environments) can become strongly associated with the experience. Later, these cues can trigger intrusion symptoms even when there is no real danger.
Because the memory is not fully contextualized, the brain responds as if the threat is occurring in the present moment.
The Role of Early Maladaptive Schemas
Early maladaptive schemas can further amplify intrusion symptoms. Trauma often reinforces schemas related to vulnerability, mistrust, or lack of control.
These schemas shape attention and interpretation, making individuals more likely to perceive threat and experience reactivation of trauma-related material (Vasilopoulou et al., 2020).
Avoidance and Suppression
Attempts to suppress or avoid trauma-related thoughts can paradoxically increase intrusion frequency. Avoidance prevents the memory from being processed and integrated, leaving it in a fragmented and easily triggered state (Wegner, 1994).
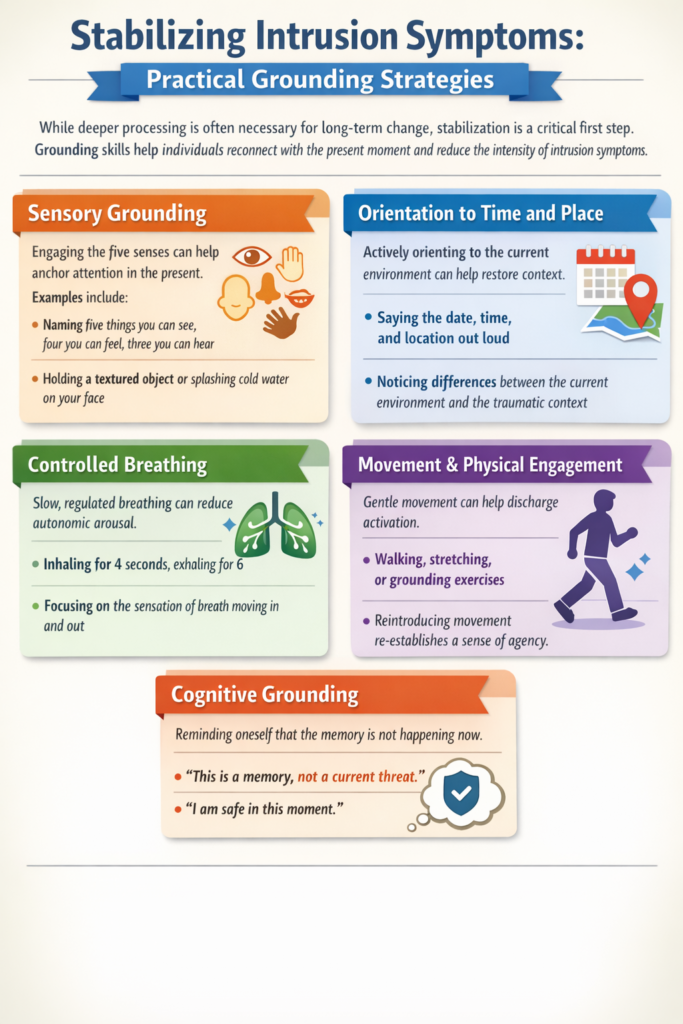
Stabilizing Intrusion Symptoms: Practical Grounding Strategies
While deeper processing is often necessary for long-term change, stabilization is a critical first step. Grounding skills help individuals reconnect with the present moment and reduce the intensity of intrusion symptoms.
Sensory Grounding
Engaging the five senses can help anchor attention in the present.
Examples include:
• Naming five things you can see, four you can feel, three you can hear
• Holding a textured object or splashing cold water on your face
These techniques counteract the sensory dominance of trauma memories by reorienting the brain to current reality.
Orientation to Time and Place
Intrusions often involve a collapse of time, where the past feels like the present. Actively orienting to the current environment can help restore context.
This might include:
• Saying the date, time, and location out loud
• Noticing differences between the current environment and the traumatic context
Controlled Breathing
Slow, regulated breathing can reduce autonomic arousal.
For example:
• Inhaling for four seconds, exhaling for six
• Focusing on the sensation of breath moving in and out
This helps signal safety to the nervous system and can reduce the intensity of emotional and physical reactions.
Movement and Physical Engagement
Gentle movement, such as walking or stretching, can help discharge physiological activation.
Trauma often involves a sense of immobilization. Reintroducing controlled movement can support regulation and re-establish a sense of agency.
Cognitive Grounding
Reminding oneself that the memory is not happening now can be helpful.
Statements such as:
• “This is a memory, not a current threat”
• “I am safe in this moment”
can support reorientation and reduce distress.
When to Seek Professional Help
Grounding strategies are important, but they are not a substitute for trauma processing when symptoms are persistent or severe.
It may be time to seek professional support if:
• Intrusion symptoms are frequent or intensifying
• There is significant distress or impairment in daily functioning
• Avoidance behaviours are increasing
• Sleep is consistently disrupted
Trauma-focused therapies are designed to help individuals safely process and integrate traumatic memories. Approaches such as trauma-focused cognitive behavioural therapy, EMDR, and schema therapy work by helping the brain reprocess the trauma so it becomes a coherent, contextualized memory rather than a fragmented, intrusive one.
Processing trauma does not mean reliving it repeatedly. Instead, it involves carefully integrating the experience so that it no longer triggers the same level of emotional and physiological activation.
We Can Help with Intrusion Symptoms
Intrusion symptoms are not a sign of weakness or loss of control. They are a predictable outcome of how the brain and nervous system respond to overwhelming experiences.
Understanding these symptoms as part of a nervous system injury can reduce shame and foster a more compassionate perspective. The same systems that produce intrusion symptoms are also capable of healing when given the right support and conditions.
With appropriate stabilization, targeted therapy, and time, intrusive experiences can become less frequent, less intense, and more integrated into a broader sense of self and life narrative. CONTACT US today as an important step in your healing journey.
References
American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (5th ed.).
Brewin, C. R. (2014). Episodic memory, perceptual memory, and their interaction: Foundations for a theory of posttraumatic stress disorder. Psychological Bulletin, 140(1), 69–97.
Brewin, C. R., Gregory, J. D., Lipton, M., & Burgess, N. (2010). Intrusive images in psychological disorders: Characteristics, neural mechanisms, and treatment implications. Psychological Review, 117(1), 210–232.
Ehlers, A., & Clark, D. M. (2000). A cognitive model of posttraumatic stress disorder. Behaviour Research and Therapy, 38(4), 319–345.
Hamilton, J. L., Brindle, R. C., Alloy, L. B., & Liu, R. T. (2018). Childhood trauma and sleep among young adults with a history of depression: A daily diary study. Frontiers in Psychiatry, 9, 673.
Vasilopoulou, E., Karatzias, T., & Hyland, P. (2020). The mediating role of early maladaptive schemas in the relationship between childhood traumatic events and complex PTSD symptoms. Journal of Loss and Trauma, 25(2).
Wegner, D. M. (1994). Ironic processes of mental control. Psychological Review, 101(1), 34–52.
Prepared by Dr. Jennifer Barbera, PhD, Registered Psychologist
Dr. Jennifer Barbera PhD, C. Psych is a licensed psychologist with over 25 years of counselling experience. She has extensive clinical expertise supporting individuals and couples with anxiety, trauma, depression, addiction, and relationship challenges. Her work combines evidence-based approaches with practical strategies to help clients build resilience and improve well-being.[/vc_column_text][/vc_column][/vc_row]